Chronic Back Pain from Sitting: When to Get an MRI Scan
You spend long hours at your desk, and by the end of the day, your lower back feels stiff, sore, and persistently uncomfortable. What starts as mild discomfort can gradually become chronic back pain that affects your work, sleep, and daily routine. At this stage, many people wonder whether they need an MRI scan for back pain or whether the issue can improve with simple measures. The decision is not always straightforward and depends on your symptoms and whether any warning signs are present.
In this blog, you will understand when imaging is necessary and when an MRI for back pain remains the right first step.
Key Takeaways:
- Most chronic back pain from sitting improves with posture correction, movement, and physiotherapy without immediate MRI.
- An MRI scan for back pain is necessary when symptoms persist or worsen, or when nerve-related signs are present.
- Red flag symptoms, such as weakness or bladder changes, require urgent imaging and medical evaluation.
Quick Answer: An MRI scan for back pain is needed if the pain lasts beyond 4-6 weeks, spreads to the leg, or includes weakness or changes in bladder function, indicating possible nerve or spinal issues.
Quick Links
Why Sitting All Day Causes Lower Back Pain
Sitting feels like the safest, most low-effort thing your body can do, but your spine tells a very different story. Prolonged sitting loads your lumbar discs unevenly and forces the muscles around your spine to work continuously just to keep you upright.
Over months and years, this creates the kind of deep, persistent lower back pain that does not go away on its own.
- Disc compression: The discs between your vertebrae act as shock absorbers. Sitting significantly increases pressure in these discs compared to standing, and sustained pressure for long hours can cause them to bulge or degenerate more quickly.
- Poor posture strain: When you lean toward your screen, the mechanical force on your lower back increases sharply. Research shows that sitting in a forward-flexed position increases the odds of developing lower back pain by more than 6 times compared to sitting upright [1].
- Muscle imbalance: Prolonged sitting causes the hip flexors to tighten and the core muscles that protect your spine to weaken. This imbalance shifts the load directly onto your spinal joints and discs, making chronic pain far more likely over time.
- Muscle fatigue: Unlike dynamic movement, sitting keeps the same muscles contracted for hours without a break. These muscles accumulate fatigue, producing the familiar dull ache that creeps in by mid-afternoon.
- Early desk-job back pain: Back pain used to be associated with older adults or heavy manual labour. Today, desk professionals in their twenties and early thirties are presenting with chronic lower back pain, largely driven by long sitting hours, poor workstation setup, and minimal physical activity outside of work.
Next, let’s evaluate what you can actually assess for your back pain with an MRI scan.
What an MRI Scan Shows in Back Pain
An MRI is one of the most detailed diagnostic tools available for investigating the spine, but understanding what it can and cannot tell you will help you use it wisely. It uses powerful magnets and radio waves to create high-resolution images of the soft tissues inside your back, all without exposing you to any radiation.
- Soft tissue detail: X-rays detect fractures and bone alignment issues, but they do not show discs, nerves, or ligaments. A lumbar MRI gives your doctor a clear view of all the structures most commonly responsible for chronic back pain.
- Disc herniation: When the soft inner material of a spinal disc pushes through its outer layer and presses on a nerve, this shows up clearly on an MRI. The scan identifies exactly which disc is affected and how severely it is compressing the surrounding nerve roots.
- Nerve compression: If pain shoots down your leg or you experience numbness and tingling, an MRI can confirm whether a compressed nerve root in your lumbar spine is responsible and pinpoint the exact level.
- Stenosis and degeneration: MRI identifies abnormal narrowing of the spinal canal, degenerative disc disease, and inflammatory changes. All of these conditions can cause persistent lower back pain and leg symptoms that need targeted treatment.
- Incidental findings: Studies show that disc degeneration appears on MRI in 20% of healthy twenty-year-olds and over 80% of healthy adults above sixty, even with no pain at all [2]. This is exactly why the decision to scan must always be made by a qualified doctor.
Also read: Can I Get An MRI With Dental Implants Or Gold Jewellery?
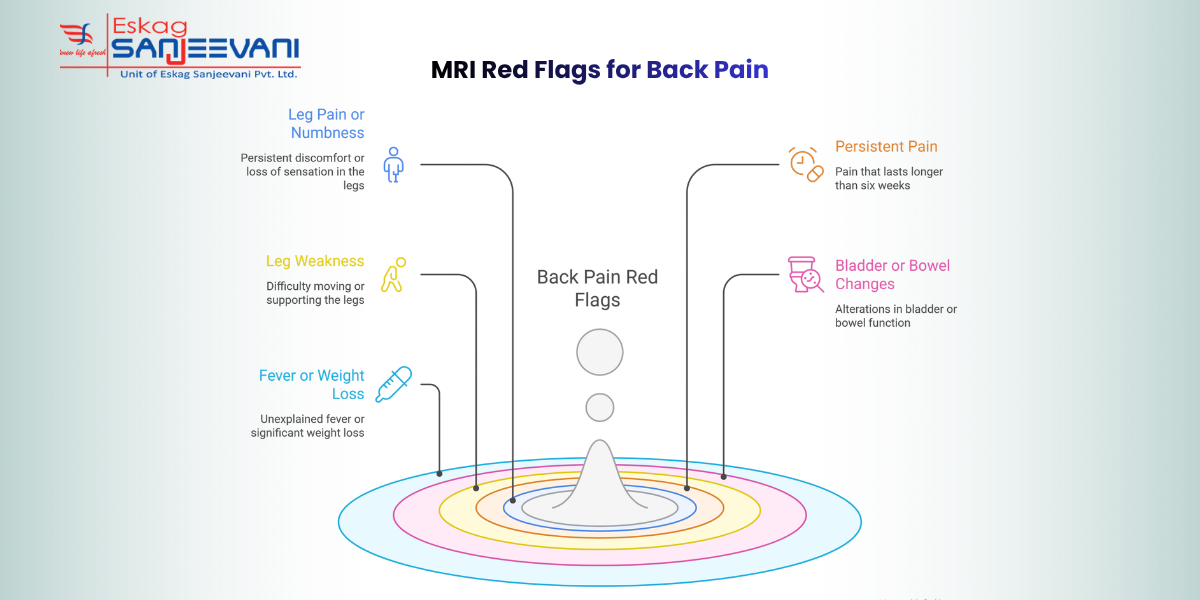
Back Pain Red Flags That Need an MRI
Most back pain from sitting is uncomfortable but not dangerous. A smaller set of symptoms serves as the body’s distress signal, indicating that something more serious may be happening within the spine. Knowing the difference between ordinary desk soreness and genuine red flags could genuinely protect your long-term health.
Recognising these red flags helps avoid delay in diagnosis and treatment.
Leg Pain or Numbness
When a spinal nerve root is compressed, most often by a herniated disc at the L4–L5 or L5–S1 level, it produces pain that travels from the lower back through the buttock and down the leg, often reaching the foot. This is sciatica, the clearest indicator of nerve involvement. An MRI of the lumbar spine is the most reliable test for confirming the cause and guiding appropriate treatment. Pain or tingling that travels past the knee, worsening leg weakness, or symptoms isolated to one side all point to a specific spinal level that MRI can precisely identify.
Persistent Pain Beyond 6 Weeks
Acute back pain, even when severe, resolves in most people within four to six weeks with conservative care. When pain persists beyond this window despite rest and over-the-counter relief, it is no longer routine. Chronic back pain lasting twelve weeks or more often signals an underlying structural issue that conservative measures alone are unlikely to resolve, and imaging gives your doctor the information needed to move treatment forward purposefully [3]. Pain that is worst at night, wakes you from sleep, or feels worse in the morning and gradually improves through the day may also point toward inflammatory rather than mechanical causes.
Leg Weakness
A sense of heaviness in the legs, foot drop, or unsteadiness when walking are not ordinary back pain symptoms; they suggest that nerve compression is beginning to affect motor function, not just sensation. Progressive motor weakness requires urgent imaging because delayed treatment can result in permanent nerve damage that is very difficult to reverse [4]. If your legs feel unreliable or your walking is becoming affected alongside back pain, do not wait to see if it passes on its own.
Bladder or Bowel Changes
A sudden change in bladder or bowel control alongside lower back pain is a medical emergency. This combination, especially when paired with numbness in the inner thighs and groin, suggests cauda equina syndrome, where the nerve bundle at the base of the spine is severely compressed. Cauda equina syndrome requires immediate MRI and emergency surgical decompression, and outcomes are significantly worse the longer treatment is delayed.
Fever or Weight Loss
When back pain is accompanied by a persistent fever, chills, night sweats, or unexplained weight loss, it suggests the spine may be affected by something beyond mechanical wear and tear. Spinal infections such as osteomyelitis or discitis require targeted medical or surgical treatment, not physiotherapy or rest, and an MRI is the fastest way to confirm the diagnosis. If you have a personal history of cancer and develop new or worsening back pain, an MRI is needed immediately to rule out metastatic disease involving the spine.
When You Do Not Need an MRI Yet
If your back pain is less than six weeks old and you have none of the red flags above, clinical guidelines from leading medical organisations do not recommend rushing to get an MRI scan. In fact, early imaging can lead to unnecessary anxiety, additional tests, and even procedures that do not benefit the patient at all.
- Physiotherapy first: Conservative care directly targets the muscle imbalances, postural strain, and disc loading that create sitting-related back pain. These approaches carry strong clinical evidence and work well when started early and followed consistently.
- Regular movement breaks: Research found that switching positions and standing up every 15 minutes significantly reduces lower back discomfort among desk workers. A simple phone reminder every hour is one of the highest-impact, lowest-cost strategies available.
- Heat therapy: Applying a warm compress to the lower back relaxes the tight muscles around the lumbar spine and reduces the muscle guarding that often makes desk-related pain feel far more severe than it actually warrants.
- Reassess at 6 weeks: If you have consistently worked on posture, movement, and ergonomics for six weeks and pain is unchanged or worsening, that is the right time to return to your doctor and have a proper conversation about imaging.
With a better understanding of when not to undergo an MRI scan, let’s understand what happens after a lumbar MRI.
What Happens After a Lumbar MRI
Getting your MRI done is not the end of the road; it is the beginning of a clearer path forward. Understanding what the scan process involves, how to read your report, and what different findings actually mean for treatment will help you leave the radiology centre feeling informed rather than overwhelmed.
- Scan process: You lie still inside the MRI machine for approximately 30 to 45 minutes while images are acquired. The machine makes loud knocking sounds, but you feel nothing, and if you have metal implants, a pacemaker, or significant claustrophobia, you must inform the radiology team before the scan begins.
- Report terms: A “disc bulge” means the disc is pressing outward but has not ruptured. A “disc herniation” means inner material has pushed through and may be touching a nerve. “Foraminal narrowing” means reduced space where nerve roots exit the spine, and “spinal stenosis” means the spinal canal has narrowed; neither of these automatically means surgery.
- Non-surgical care: The majority of people diagnosed with disc herniation or nerve compression improve significantly with physiotherapy, anti-inflammatory medication, and targeted exercises. Surgery is reserved for cases where conservative treatment has genuinely failed or where motor function is at progressive risk.
- Clinical correlation: A large disc bulge in someone with minimal symptoms may need only monitoring and lifestyle changes. A smaller herniation causing significant nerve symptoms and leg weakness may need active treatment; imaging findings alone never determine the treatment plan.
If your doctor has advised an MRI for back pain, prompt, precise imaging makes a real difference in how quickly treatment can begin. If you are looking for the best MRI centre near you, Eskag Sanjeevani Radiology offers 1.5 Tesla (T) and 3T high-resolution lumbar MRI with same-day reporting. Close coordination with your treating doctor and a patient-first approach ensures your results are clearly communicated and clinically useful from the start.
Also read: What Your Radiology Test Results Really Mean (Explained Simply)
Final Thoughts
Chronic back pain from prolonged sitting often improves with posture correction, movement, and guided physiotherapy when addressed early and consistently. However, persistent pain, nerve-related symptoms, or functional changes require timely clinical evaluation and, if advised, an MRI scan for back pain to identify the exact cause. Acting early prevents complications and supports better long-term outcomes.
At Eskag Sanjeevani Radiology Centres, MRI services focus on accurate imaging, prompt reporting, and coordination with your treating doctor, so your next step is based on clear evidence rather than guesswork.
References
- Lis, A.M., Black, K.M., Korn, H. and Nordin, M. (2006). Association between sitting and occupational LBP. European Spine Journal, [online] 16(2), pp.283–298.
- INSIGHTS, N., 2011. MRIs Should Be Used Sparingly in Patients With Low Back Pain. journal of orthopaedic & sports physical therapy, 41(11), p.847.
- Lancaster, B., Goldman, J., Kobayashi, Y. and Gottschalk, A.W. (2020). When Is Imaging Appropriate for a Patient With Low Back Pain? Ochsner Journal, 20(3), pp.248–249.
- Humphreys, S.C., Eck, J.C. and Hodges, S.D. (2002). Neuroimaging in Low Back Pain. American Family Physician, [online] 65(11), pp.2299–2307.
Intermittent back pain that fully resolves between episodes, has no leg involvement, and does not affect daily function generally does not need an MRI. If episodes are becoming more frequent or intense, consult a doctor to assess whether imaging is appropriate.
Not always. Some patients with genuine back pain have structurally normal MRI scans because pain can stem from muscle dysfunction or nerve sensitisation that imaging does not capture clearly. MRI is one part of a broader diagnostic picture that includes clinical examination.
Yes. MRI does not use ionising radiation, making it safe for repeated clinical use. Patients with pacemakers, certain metal implants, or cochlear devices should inform the radiology team before scanning so safety checks can be completed appropriately.
A lumbar MRI focuses on the lower five vertebrae, which are responsible for most desk-related pain and sciatica. A full-spine MRI covers all three spinal regions and is ordered only when symptoms suggest involvement across multiple levels, which is uncommon in sitting-related back pain.
In the vast majority of cases, no. Most findings, including disc bulges and mild nerve compression, respond well to physiotherapy and conservative care. Surgery is considered only when symptoms are severe, progressive, or unresponsive to an adequate non-surgical treatment trial.
Look for a centre with high-resolution MRI technology, fast reporting, and direct coordination with your treating doctor. If you are searching for the best MRI centre near you, Eskag Sanjeevani Radiology Centres offer 1.5T and 3T lumbar MRI with same-day reporting and experienced musculoskeletal radiologists.

