Mammogram vs USG: The Ultimate Breast Cancer Scan Guide
Breast cancer is the most common cancer among women in India, and an early, accurate diagnosis can genuinely change the outcome of treatment.
Many women feel uncertain about whether to get a mammogram or a USG breast test, and that uncertainty often leads to delayed screening. Both scans serve distinct clinical purposes; neither replaces the other, and choosing the wrong scan for your age or breast type can lead to a missed finding. Understanding the difference between a breast test, a mammogram and a USG breast test is not a clinical question reserved for doctors; it is information every woman deserves to have.
In this blog, you will find a clear, evidence-based comparison of both scans, clinical breast examination steps, and practical guidance on when to act.
Key Takeaways:
- A mammogram detects early breast cancer changes like calcifications, while USG helps assess dense breast tissue and masses.
- Both tests serve different roles and are often used together for accurate breast cancer screening.
- A clinical breast examination helps determine the appropriate imaging test based on symptoms, age, and risk factors.
Quick Answer: A mammogram uses low-dose X-rays to detect early breast cancer changes; a USG uses sound waves to examine breast tissue in detail. Both are breast cancer scans that work best together.
Quick Links
What Is a Breast Cancer Scan?
A breast cancer scan is any imaging test used to detect abnormal tissue changes before or after symptoms appear. The right scan, used at the right time, is one of the most effective tools for early detection.
Two primary imaging tools exist, mammography and ultrasonography (USG), and each serves a distinct clinical role based on your age, breast density, and symptoms. All breast imaging results are reported using the BI-RADS system (categories 0–6), which gives your radiologist a standardised framework to guide next steps after your breast test.
Mammogram Test: How It Works
A mammogram is a low-dose X-ray of the breast that detects cancerous changes, including calcifications, years before a lump becomes physically noticeable. It is the only breast cancer scan with clinical trial evidence of reducing breast cancer mortality. During the procedure, the breast is compressed between two surfaces to capture clear images from two angles. The compression lasts only a few seconds and may cause mild temporary discomfort.
- Detects calcifications, the earliest sign of breast cancer, invisible on USG.
- Identifies asymmetries and structural tissue changes across the whole breast.
- Detects Stage 0 (non-invasive) breast cancer, which USG frequently misses.
- Provides a year-on-year tissue map for comparison at follow-up scans.
- Achieves 85-90% accuracy as a standalone breast cancer scan [1].
- Dense breast tissue and cancerous tissue both appear white on the image, reducing sensitivity in younger women.
- Involves a small radiation dose, though well within internationally accepted safe limits.
In India, the Breast Imaging Society of India (BISI) recommends mammography from age 30 for symptomatic women, lower than the age 40 threshold in Western guidelines, given the earlier age of breast cancer onset in Indian women [2].
USG Breast Test: When Is It Needed?
A USG breast test uses high-frequency sound waves to produce real-time images of breast tissue without radiation or compression. It is the preferred first-line breast cancer scan for younger women, pregnant women, and those with dense breast tissue where mammography has reduced sensitivity.
A handheld transducer moves across the breast surface, and sound waves bounce off internal structures to create images on a monitor. The procedure is painless, involves no radiation, and is safe at all ages, including during pregnancy.
- Distinguishes fluid-filled cysts (typically benign) from solid masses (potentially malignant), a distinction mammography cannot reliably make.
- Examines dense breast tissue with higher sensitivity than mammography in women under 45 [3].
- Assesses axillary lymph nodes for signs of cancer spread.
- Guides needle biopsy procedures with real-time imaging precision.
Cannot detect calcifications, the earliest and most reliable marker of breast cancer. - Results are operator-dependent and vary with the sonographer’s skill and experience.
- Not proven as a standalone screening tool for reducing breast cancer mortality.
To choose the right breast cancer screening test, it is important to compare mammograms and USG in terms of purpose, accuracy, and clinical use.
Mammogram vs USG: Key Differences
Mammogram and USG breast tests are complementary tools; the clinical question is never one versus the other, but which scan to use first and when to use both together. When combined, they detect approximately 2-3 additional breast cancers per 1,000 women compared to mammography alone [4].
Here is a tabular representation of the difference between a mammogram and a USG:
| Feature | Mammogram | USG Breast Test |
| Technology | Low-dose X-ray | High-frequency sound waves |
| Radiation | Yes (very low, safe dose) | None |
| Recommended age (India) | 30+ symptomatic; 40+ screening | Under 30; all ages as a supplement |
| Dense breast performance | Reduced sensitivity | Higher sensitivity |
| Detects calcifications | Yes, primary strength | No |
| Distinguishes cyst vs mass | Limited | Yes, primary strength |
| Breast compression | Yes | No |
| Procedure comfort | Mild, temporary discomfort | Painless |
| Standalone screening role | Proven | Supplementary only |
| Proven mortality benefit | Yes | Not established alone |
Also read: USG Scan in Pregnancy: A Simple Guide for Indian Parents.
Before any breast cancer scan, a clinical breast examination helps identify early signs and guides the most appropriate imaging approach for you.
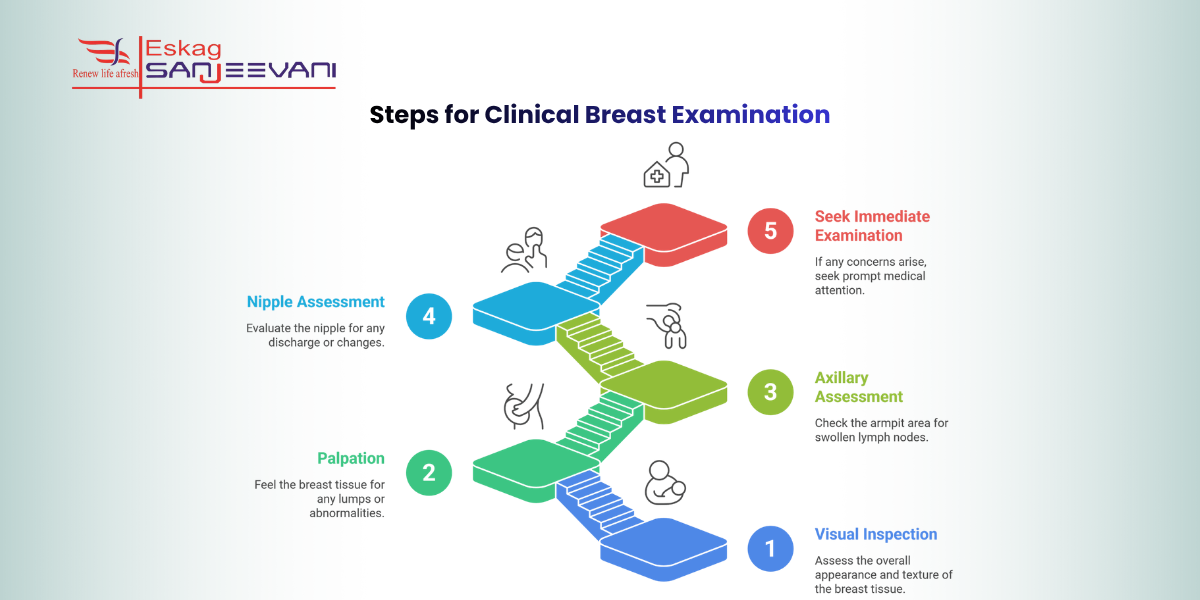
Clinical Breast Examination Steps
A clinical breast examination (CBE) is a physical assessment by a trained doctor to detect lumps, skin changes, or nipple abnormalities before any imaging is ordered. It is the clinical starting point that determines which breast cancer scan, mammogram, USG, or both, is most appropriate for you.
In India, CBE is recommended every 1-3 years for women aged 20-39 and annually from age 40, and it should always precede or accompany imaging decisions.
Visual Inspection and Palpation
The doctor begins with a visual check of both breasts for skin dimpling, nipple changes, asymmetry, or visible lumps. This is followed by systematic palpation of the entire breast in a circular or vertical pattern to identify any thickening, texture change, or discrete mass. Both steps together provide the initial clinical picture that informs all further breast examination decisions.
Axillary and Nipple Assessment
The axillary (armpit) lymph nodes are examined for enlargement, which may indicate regional spread of cancer beyond the breast. The nipple is assessed for any discharge, retraction, crusting, or surface changes that may not yet be visible on a scan. These findings, when combined with palpation results, help your doctor decide whether an immediate breast test or breast cancer scan is needed.
When to Seek an Immediate Breast Examination
A CBE becomes urgent when specific warning signs are present. These include a new lump in the breast or armpit, skin dimpling or puckering, nipple discharge or inversion, changes in breast shape or symmetry, and persistent focal breast pain that does not resolve with the menstrual cycle. A normal CBE does not eliminate the need for imaging; many early-stage cancers remain clinically undetectable on physical examination alone.
Final Thoughts
If you notice any change in your breast, a lump, skin change, or nipple discharge, do not wait for your next routine check to seek a breast cancer scan. Start with a clinical breast examination, as this guides your radiologist toward the most appropriate imaging for your age and symptoms. For women over 40, a mammogram every one to two years remains the most evidence-based step you can take for early detection.
For younger women or those with dense breast tissue, discuss a USG breast test with your doctor before symptoms develop, and choose a dedicated scan centre with radiologists experienced in breast imaging for the most accurate results. The team at Eskag Sanjeevani Radiology centres provides protocol-driven imaging so that when you come in with a concern, you leave with a clear clinical answer.
References
- Cleveland Clinic. (2024). Mammogram vs. Breast Ultrasound: Which One Is Best? [online] Cleveland Clinic.
- Chakrabarthi, S., Panwar, S., Singh, T., Lad, S., Srikala, J., Khandelwal, N., Misra, S. and Thulkar, S. (2022). Best Practice Guidelines for Breast Imaging, Breast Imaging Society, India. Annals of the National Academy of Medical Sciences (India).
- Devolli-Disha, E., Manxhuka-Kërliu, S., Ymeri, H. and Kutllovci, A. (2009). Comparative Accuracy of Mammography and Ultrasound in Women with Breast Symptoms According to Age and Breast Density. Bosnian Journal of Basic Medical Sciences, 9(2), pp.131–136.
- Cohen, E. (2024). Mammogram vs. breast ultrasound: What’s the difference? [online] MD Anderson Cancer Centre.
A mammogram uses low-dose X-rays and is best for detecting calcifications and early-stage breast cancer in women over 30. A USG breast test uses sound waves, involves no radiation, and excels at examining dense breast tissue and distinguishing cysts from solid masses.
CBE should begin at age 20. For symptomatic women in India, mammography is recommended from age 30. Screening mammography for average-risk women typically begins at age 40, or earlier for those with a family history of breast cancer.
No. USG cannot detect calcifications and has no standalone evidence of reducing breast cancer mortality. It works best as a supplement to mammography, not a replacement.
For average-risk women over 40, a mammogram every one to two years is generally recommended. Women with elevated risk should follow individualised guidance from their doctor or radiologist.
An abnormal result does not confirm the presence of cancer. It means further assessment is needed, a diagnostic mammogram, additional USG, or, in some cases, a biopsy. Your radiologist will guide the next steps based on your BI-RADS category.


 Medically Reviewed
Medically Reviewed